The Big Squeeze
New approaches to managing reimbursements for pharmacy benefit programs are testing Big Pharma.
US drug manufacturers face significant risks from a trend toward a more controlled approach to the operation of pharmacy benefit networks (PBNs) that deliver medicines to patients. Instead of letting patients choose to fill their prescriptions from an open network that includes a wide range of pharmacies, these benefit designs use financial incentives or explicit restrictions to direct consumers to specific pharmacies that agree to meet the PBN's conditions. The popularity of these new pharmacy network models is exploding in both commercial and Medicare Part D plans.

Getty Images/Tim Teebken
The risk is the shift in the balance of power to payers in the decisions on if, how, and when patients get access to medicines provided under their pharmacy benefit plans. These so–called narrow networks will give more control to third-party payers, alter promotion and marketing activities, and shift market share between different payers and pharmacies. Payers' use of the more tightly controlled pharmacy network model will keep growing as they seek additional drug spending savings. Over the past two years, plans have taken further steps to enforce formulary control and limit manufacturer marketing practices, such as copay offset programs. More important, consumers are accepting the new plans, encouraged by the out-of-pocket savings opportunities on their prescriptions. Likewise, community retail pharmacies are willing to accept lower reimbursements in exchange for the increased store traffic.
To preserve market position and access, manufacturers must start by recognizing that the economic interests of payer-defined pharmacy channels are diverging from traditional branded drug makers. It is thus important to analyze this crucial trend, highlight its economic appeal to payers and pharmacies, and outline how manufacturers can best prepare for and respond to the challenge.
A crucial distinction
For consumers with third-party insurance, pharmacy benefit managers (PBMs) assemble networks of pharmacies. In an open pharmacy network, a consumer's out-of-pocket costs and copayments are identical regardless of which pharmacy in the retail network dispenses the prescription.
An open pharmacy network, which remains the most common network design, includes nearly all of the approximately 62,000 US retail pharmacies. Network pharmacies compete on service, convenience, and location to attract consumers within a particular plan. Under this approach, there are no financial incentives for a consumer with third-party coverage (and a flat copayment) to shop at the pharmacy with the lowest cost per prescription for the payer.
Today, payers are rapidly adopting networks that differ significantly from the traditional open network design. More than four out of 10 seniors are now enrolled in a Medicare Part D Prescription Drug Plan (PDP) with a narrow pharmacy network design. A survey by the Pharmacy Benefit Management Institute reports that one out of five employers have started utilizing narrow networks. For instance, more than 1,000 commercial plans with 14.5 million covered lives use the Maintenance Choice narrow network program of retail chain and PBM CVS Caremark. Walmart, the third-largest retail pharmacy, estimates that nearly 25 percent of its 2012 prescription volume derived from its participation in narrow networks, compared with less than 1 percent in 2009.
There are two types of narrow networks. A preferred network gives the consumer a choice of pharmacy, but gives consumers financial incentives to use the particular pharmacies that offer lower costs or greater control to the payer. In other words, a consumer with a preferred network benefit design retains the option of using any pharmacy in the network. However, the consumer's out-of-pocket expenses will be higher at a non-preferred pharmacy.
One of the first commercial preferred retail networks was the trial program between Walmart and Caterpillar, which began in September 2008. As part of the pilot program, 70,000 Caterpillar beneficiaries (employees, retirees, spouses, and dependents) had a $0 copayment on 2,500 "tier 1" (lowest priced) generic drugs that are filled at any Walmart pharmacy. However, the copayment was $5 if the beneficiary chose to fill a prescription for one of these drugs at any other pharmacy in the network. Caterpillar has subsequently broadened its preferred network to include Walgreens, Kroger, and a group of independent pharmacies.
Medicare Part D beneficiaries, for example, annually choose their own new plan, rather than having a benefit administrator or insurance plan provide a few choices for them. Thus, preferred network adoption directly demonstrates consumer appeal. According to the Center for Medicare and Medicaid Services (CMS), preferred pharmacy networks are permitted under the law that created the Medicare Part D benefit.
Table 1 highlights the largest payers that sponsor Part D prescription drug plans. In plans administered by such large payers as UnitedHealth and Humana, the vast majority of seniors are now enrolled in plans with preferred networks. For the 2013 benefit year, plans with preferred pharmacy networks enrolled 9.5 million people, or 42 percent of the total 22.4 million seniors in a Medicare PDP.
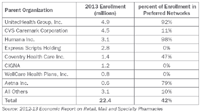
Table 1: Enrollment in Medicare Part D PDPs, by parent organization, January 2013.
The Humana Walmart-Preferred Rx Plan illustrates the popularity and rapid adoption of this network model. In October 2010, Walmart and Humana launched this PDP with 4,200 preferred pharmacies (including Walmart, Sam's Club, Neighborhood Market, and Humana's RightSource mail pharmacy) and 58,000 non-preferred retail pharmacies. In 2013, Humana Walmart-Preferred Rx Plan is the fourth-largest PDP, with 7.8 percent of total PDP enrollment. Compared to 2012, total enrollment grew by 355,279 seniors (+25.5 percent).
The second type of narrow network is a limited pharmacy network. This more restrictive model designates the particular pharmacies or dispensing formats available to a patient when filling her prescription. A limited network gives a payer the greatest degree of economic control over prescription fulfillment. Payers will include only those pharmacies with the lowest costs of dispensing and/or the highest service levels. In exchange, the pharmacy becomes one of the selected members in the network and increases its market share.
A typical limited retail pharmacy network is 50 percent to 80 percent smaller than an open network. Thus, the consumer can choose any pharmacy within the network, but the network has only 10,000 to 30,000 pharmacies (versus more than 60,000 total retail pharmacies). An example is Restat's Align network, which includes national chains (Walmart, Target, and many supermarkets) and a number of regional chains. In 2013, Express Scripts, the largest PBM, launched the Express Advantage Network, a limited network with about 20,000 pharmacies. Payers also establish limited networks for specialty drugs by restricting pharmacy choice to just one or two payer-designated specialty pharmacies.

Figure 1: The number of participating pharmacies in narrow retail pharmacy networks broken down by category.
Mandatory mail benefit designs are the most common application of limited networks. They require consumers to fill 90-day prescriptions through a mail pharmacy without the option of using a retail pharmacy. About 25 percent of employers require that some or all maintenance medications be dispensed by a mail pharmacy.
CVS Caremark's Maintenance Choice program is the most prominent limited network model for commercial plan sponsors. Under the Maintenance Choice program, a beneficiary can obtain maintenance medications from a CVS retail pharmacy or a CVS Caremark mail pharmacy. This model lets consumers choose the pharmacy channel (mail or retail) but limits that choice to CVS Caremark outlets.
With the exception of the Maintenance Choice model, limited networks have been much less widely adopted than preferred networks. We speculate that commercial plan sponsors may believe there are bigger savings opportunities in other areas that have less potential beneficiary disruption, such as increasing cost-sharing requirements.
Rationale for going narrow
Many interrelated factors are supporting the adoption of narrow networks:
» Plan sponsors save money with narrower networks. An independent analysis conducted for the PBM Restat concluded that an employer would achieve savings of four percent to 13 percent. Walmart claims that employers achieve average savings in the 13 percent to 18 percent range from its limited network models, but savings can go as high as 45 percent. CVS Caremark recently stated that its limited Maintenance Choice model will save payers four percent of drug spending. Almost one out of five Managed Medicaid plans now uses a limited network, driven by intense cost pressure due to state government shortfalls.
» Consumers have access to many alternative community retail pharmacy outlets. More than nine out of 10 Americans live within five miles of a retail pharmacy. Consumers in a core based statistical area (CBSA)—an urban center of at least 10,000 people and its adjacent areas—live within 1.2 miles of a community retail pharmacy. In many major metropolitan markets, up to 50 percent of market share is held by pharmacies beyond the largest four retail chains—CVS/Pharmacy, Walgreens, Walmart, and Rite Aid. Given the ready availability of pharmacy outlets, plans can establish narrower networks with minimal consumer disruption.
» Consumers are willing to switch pharmacies to reduce out-of-pocket expenses. A preferred or limited network causes the consumer some degree of inconvenience. However, surveys demonstrate that consumers are willing to shift pharmacies for even very small monetary rewards. In a recent national survey, 85 percent of consumers said they would switch pharmacies to avoid higher copayments at their usual pharmacy.
» Pharmacies are willing to boost store traffic in exchange for accepting lower prescription reimbursements. Since overall prescription growth remains very low, pharmacies are trying to remain competitive and attract consumers in a relatively saturated market. Consequently, they have been willing to accept reduced reimbursement rates in exchange for participation in a preferred or limited network. A majority of these savings comes from reduced pharmacy margins, because pharmacies compete to be in a payer's narrower network.
» Narrow networks are consistent with broader healthcare insurance models. Insurance plans have long used preferred provider models for medical services. Many use tiered network models that categorize medical providers in the network based on quality, cost, and/or the efficiency of the care they deliver. These networks encourage patients to visit more-efficient doctors—either by restricting networks to certain providers or by having different copayments or coinsurance for providers in different tiers in the network. In 2011, 20 percent of employers that offered health benefits included a high performance or tiered provider network in the health plan with the largest enrollment.
» A dispute between Express Scripts and Walgreens demonstrates the viability of a limited network model. In January 2012, Walgreens exited PBM Express Scripts' retail pharmacy network. Walgreens' prescription sales declined sharply, but the effect on Express Scripts' PBM business was minimal. A small number of plan sponsors switched away from Express Scripts to keep Walgreens in their network, but most accepted the narrower network. After the September 2012 resolution of the Walgreens-Express Scripts dispute, such plan sponsors as the Department of Defense's TRICARE program and Blue Cross of Idaho declined to add Walgreens back to their networks.
Impact on manufacturers
The "narrow network revolution" will affect pharmaceutical manufacturers' commercial activities, in the following ways:
» Narrow networks give more control to third-party payers. Today, a pharmacy's participation in a payer's narrow network is based primarily on the pharmacy's willingness to accept reduced reimbursements. As these networks become more common, payers will begin considering additional selection criteria linked to a pharmacy's compliance with a payer's benefit management plan. For example, payers could select pharmacies with higher generic substitution rates or a greater willingness to block copay cards.
» Narrow networks shift market share between payers. When negotiating for formulary access, manufacturers should be aware how payers can leverage new network models to gain market share. In October 2010, Walmart and Humana launched this PDP with 4,200 preferred pharmacies (including Walmart, Sam's Club, Neighborhood Market, and Humana's RightSource mail pharmacy) and 58,000 non-preferred retail pharmacies. As of 2013, the plan is the fourth-largest PDP in the United States, with about 8 percent of all Part D enrollees.
» Narrow networks shift market share between trading partners. Existing programs can be disrupted or altered as networks evolve. When Walgreens exited the Express Scripts network, rival pharmacies gained from Walgreens' sales losses. Until September 2012, year-over-year sales declined by 10 percent to 15 percent at Walgreens pharmacies, while sales increased at the other chains. CVS's retail pharmacies gained 6.5 million to 7 million new prescriptions from former Walgreens' customers. It expects to retain 60 percent of these customers. Many other pharmacies also reported picking up new business from defecting Walgreens' customers.
» Narrow networks teach consumers to shop for prescriptions by price. Thanks to prescription drug insurance, US consumers' out-of-pocket expenses—cash-pay prescriptions plus copayments and coinsurance—account for less than 20 percent of total US outpatient prescription drug spending. Historically, consumers have considered only service and location when choosing a pharmacy. Narrow networks ask consumers also to consider which particular pharmacy has the lowest out-of-pocket cost. This trend accentuates consumers' price sensitivity for prescriptions.
Three ways to respond
Narrow retail pharmacy networks are created by payers for payers, with the patient coming in second. Thus, pharmaceutical manufacturers have a very limited ability to influence the adoption of this new design. However, companies should take action to understand and prepare for the ongoing growth of these networks.
» Build cross-organizational insight. Narrow networks challenge conventional organizational arrangements within most pharmaceutical manufacturers. This can make it harder to spot brand-specific sales implications of narrow networks. Usually, the trade function that manages pharmacy distribution channel relationships is organizationally separate from the managed markets function that interacts with payers. Functions that handle payer relationships, such as managed markets and payer marketing, must understand the product movement and payment functions, and vice versa. For instance, are copay offset programs being blocked with greater frequency in certain networks? Is patient access being compromised or affected by a payer's adoption of this new network model?
» Be prepared to alter promotion plans. As new pharmacy network models proliferate, patients will begin moving prescriptions from one pharmacy to another. In some cases, these shifts will require changes to traditional geographic promotion planning activities. For example, membership-warehouse club retailer Costco operates Costco Health Solutions (CHS), a pharmacy benefit manager targeting self-insured employers located near Costco stores. These employers are encouraged to set up a preferred network model, in which the beneficiary has a financial incentive to choose a Costco pharmacy to reduce the employer's drug costs. This movement may or may not correspond to existing sales and marketing plans. Sales teams should understand managed care coverage and new retail provider networks so they can have meaningful discussions with practices and tailor messages accordingly.
» Develop a coherent policy position. Manufacturers should be prepared to manage divergent opinions generated by the narrow network trend. Payers support narrow networks, while many pharmacies oppose them. For instance, the National Community Pharmacists Association (NCPA), which represents owners of independent pharmacies, has claimed that preferred network PDPs in Medicare Part D are being "deceptively marketed to patients and lack adequate pharmacy access for rural Americans." While no objective data yet support these assertions about patient access, the sentiment has already led to pharmacy-led lawsuits against CMS. In contrast, larger pharmacy chains are active participants in the new networks. Balancing these competing perspectives is difficult as payers and dispensing channel consolidate.
The narrow network revolution is accelerating—its time is now. Pharmaceutical manufacturers have no choice but to prepare for the coming changes in product and consumer access.
Adam J. Fein, PhD, is president of Pembroke Consulting, Inc., and CEO of Drug Channels Institute. This article is adapted from his new "2012–13 Economic Report on Retail, Mail, and Specialty Pharmacies," which is available at http://bit.ly/VnqMzt. He can be reached at afein@pembrokeconsulting.com.

The Misinformation Maze: Navigating Public Health in the Digital Age
March 11th 2025Jennifer Butler, chief commercial officer of Pleio, discusses misinformation's threat to public health, where patients are turning for trustworthy health information, the industry's pivot to peer-to-patient strategies to educate patients, and more.
Navigating Distrust: Pharma in the Age of Social Media
February 18th 2025Ian Baer, Founder and CEO of Sooth, discusses how the growing distrust in social media will impact industry marketing strategies and the relationships between pharmaceutical companies and the patients they aim to serve. He also explains dark social, how to combat misinformation, closing the trust gap, and more.